Cauda Equina Syndrome Case File
Eugene C. Toy, MD, Andrew J. Rosenbaum, MD, Timothy T. Roberts, MD, Joshua S. Dines, MD
CASE 26
A 43-year-old obese man presents to the emergency department (ED) with complaints of 12 hours of right leg pain and “tingling” in his left foot. Yesterday he was helping his neighbor carry a sofa up a flight of stairs when he experienced sudden “lightning-like” pain in his back that radiated down his legs. He went home and took acetaminophen before bed. This morning, he awoke with worsening back and left leg pain, and he was startled to notice weakness in his left foot and ankle. Now, in the ED, he reports an almost complete inability to move his left foot and a burning, constant pain throughout both legs. Physical exam reveals decreased motor strength in his left lower extremity, notably 2/5 extensor hallucis longus and foot dorsiflexor strength. He is unable to plantar flex this foot. His left hip and knee extensors are 5/5 in strength, as are all major muscular groups of his right lower and bilateral upper extremities. He has normal patellar reflexes bilaterally, but an Achilles reflex is only present on his right side. Sensation testing demonstrates decreased sensitivity to light touch and pin-prick stimulation in the perianal regions, perineum, and posterior thighs, bilaterally. The dorsum and plantar aspects of the left foot are similarly insensate. Digital rectal examination demonstrates decreased tone, and the patient is surprised to learn that his underwear is damp with urine. Bladder scan demonstrates a retained volume of 1100 mL. Vascular examination reveals warm and well-perfused skin with palpable dorsalis pedis pulses bilaterally.
► What is the most likely diagnosis?
► What are some of the most common causes of this condition?
► What are the next steps in the management of this patient?
ANSWER TO CASE 26:
Cauda Equina Syndrome
Summary: This is a 43-year-old man who presents with a 12-hour history of progressively worsening lumbosacral back and left leg pain, weakness, and sensory loss that began after he tried to lift a heavy object. He is experiencing bilateral lower extremity and perianal paresthesias, with significant weakness in his left lower extremity, diminished left-sided reflexes, decreased rectal tone, and urinary retention.
- Most likely diagnosis: Cauda equina syndrome (CES) secondary to herniated nucleus pulposis (HNP), most likely at the L4-5 level.
- Most common causes: Compression of the cauda equina secondary to lumbar disc herniation, primary tumors or metastatic disease, infections, stenosis, hematomas, and ischemic insult.
- Management of CES: Pain control, placement of urinary catheter, MRI of lumbosacral spine to confirm diagnosis and to identify region of compression, and, if positive, emergency surgical decompression of cauda equina.
ANALYSIS
Objectives
- Recognize the presentation of cauda equina syndrome (CES).
- Understand the anatomic and pathophysiologic bases of this condition.
- Be familiar with the management of CES and understand its outcomes.
Considerations
Low back pain is one of the most common complaints in EDs and primary care offices in the United States. Although back pain is disconcerting, even debilitating, to patients, very few patients presenting with acute-onset pain—0.05% by some estimates—require urgent operative intervention. CES is one such urgent indication. This patient’s symptoms, although mild at first, rapidly developed into a syndrome including sciatica, lower-extremity sensorimotor loss, and bowel and bladder dysfunction. This rapid progression of symptoms demands urgent and careful attention by knowledgeable physicians, as delayed intervention can result in devastating consequences if left untreated for greater than 24 to 48 hours.
After adequate pain relief, a complete and thorough medical history should assess for factors that make the patient prone to cauda equina, such as a history of symptoms of radicular disease, previous spinal surgery or injections, trauma, infection, the use of anticoagulants, or previous spine pathology. Potential spine fractures should be ruled out, because this patient’s symptoms began as he was undergoing significant axial loads that may have caused vertebral fractures with cord compression. Next, a thorough physical exam should be performed and must include the often-neglected assessment of sensation, motor, and reflexive function of the perianal and rectal regions, including evaluating the presence or absence of normal tone. For detailed instruction on performing the spinal exam, please refer to the “Approach to the Orthopaedic Patient” section, located near the beginning of this text.
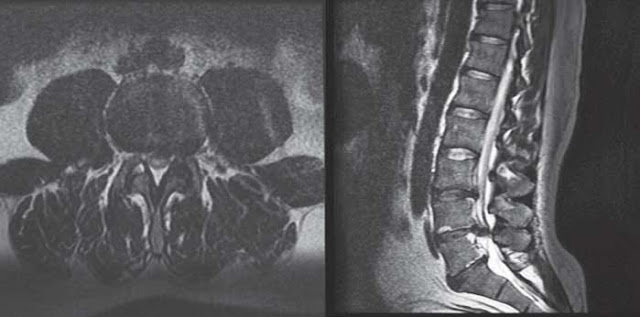
Figure 26–1. Axial (left) and sagittal (right) slices of T2-weighted spinal MRI of large, centrally herniated disc at L4-5. (Courtesy of Timothy T. Roberts, MD)
The next step in this patient’s workup includes urgent acquisition of appropriate imaging, either through magnetic resonance imaging (MRI) of the lumbosacral spine or computed tomography (CT) myelography in the presence of contraindications to MRI. MRI serves to elucidate the cause and location of the cauda equina compression, as well as to guide the surgical approach (anterior or posterior) and the need for potential arthrodesis (in the setting of instability attributable to trauma, infection, or tumor). In this case, axial and sagittal T2-weighted images, seen in Figure 26–1 , demonstrate a large, posteriorly herniated disc at the L4-5 level extruding paracentrally and laterally on the left side. Roots caudal to this level show varied levels of dysfunction consistent with midline compression of the descending lumbosacral roots. Plans should be made for urgent passage to the operating room, as permanent neurologic damage may result from delayed decompression of the cauda equina.
APPROACH TO:
Cauda Equina Syndrome
DEFINITIONS
SCIATICA: A referred pain syndrome in the buttock, leg, and/or foot distributions of the sciatic nerve, caused by compression of either the sciatic nerve itself, or its individual lumbosacral roots.
ANAL WINK REFLEX: A normal reflex of anal sphincter contraction, elicited by stroking the skin lateral to the anus. Absence of this reflex may suggest dysfunction of the S2-4 nerve roots.
LOWER MOTOR NEURON LESION: Any lesion that disrupts the function of the motor nerve fibers between the anterior horn of the spinal cord and its innervated muscles. Characterized by hypotonia, hypo- or areflexia, flaccid paralysis or weakness, fibrillations, and fasciculations. By contrast, upper motor neuron lesions affect motor nerve pathways between the cerebral motor cortex and the spinal cord and are characterized by hypertonia, hyperreflexia, and spastic paralysis.
CLINICAL APPROACH
CES is an uncommon and relatively rare condition that accounts for fewer than 1 in 2000 patients who present with lower back pain. This condition is associated with a large space-occupying lesion within the lumbosacral spine that impinges on the loose terminal roots of the spinal nerves within the spinal canal. These roots form the cauda equina, or “horse’s tail” in Latin, so named for their likeness to the equine appendage. Diagnostic criteria for CES include 1 or more of the following: (1) bladder and/or bowel dysfunction—typically retention in its early stages, (2) reduced sensation in the saddle area, or (3) sexual dysfunction, with possible motor/sensory/ reflex deficit in the lower limb. Signs and symptoms of CES develop in less than 24 hours from a given insult in more than 85% of reported cases. Nerve root compression in CES most commonly results from a herniated lumbar disc, but is thought to represent only 1% to 6% of all operative lumbar HNP cases. Risk factors for HNP include obesity, male sex, age greater than 40 years, and history of spine disorders. Less common etiologies of CES include compression by a tumorous growth, infection and abscess formation, spinal stenosis, hematoma formation, and inflammation.
Anatomy and Pathophysiology
The pathophysiology of CES is complex and not fully understood. In adults, the spinal cord terminates between the L1 and L2 vertebrae body, below which the cauda equina descend as a collection of peripheral nerve roots to the L1 to coccygeal levels. These roots are thought to be especially vulnerable to compression because they are only protected by a single layer of endoneurium, whereas most other peripheral nerves and indeed the spinal cord itself are surrounded by an epineurium, perineurium, and endoneurium. Compression and damage to the cauda equina can lead to diffuse lower motor neuron lesions, resulting in uni- or bilateral sciatica, lower extremity weakness, saddle anesthesia (resulting from insult to the S2-4 roots), and bowel and bladder dysfunction (also primarily the S2-4 roots).
Patients presenting with back pain and bowel or bladder dysfunction should raise immediate flags for the possibility of CES. Neurogenic bladder dysfunction, characterized by urinary retention more often than incontinence, is an essential symptom of CES. In normal urinary bladder physiology, the detrusor urinae muscle is responsible for contracting the bladder during voiding and is controlled by the parasympathetic nervous system (PNS) via S2, S3, and S4 nerve roots. During urinary voiding, the PNS directs detrusor contraction with simultaneous relaxation of the internal urinary sphincter. When damage to the S2-4 nerve roots occurs, the bladder cannot contract or release through the sphincter, and thus overflow incontinence develops. Postvoid residual volume should be obtained in patients in whom CES is suspected.
The S2-4 nerve roots also provide sensation to the saddle region, including the perineum, buttocks, and posteromedial thighs. A complete rectal examination, including testing for an anal wink reflex and a bulbocavernosus reflex, should be performed on CES patients. Patients presenting with both saddle anesthesia and urinary incontinence—suggestive of extensive insult to the sacral roots—have been found to have poor prognosis with regard to long-term bladder function.
Radiologic Evaluation
After a thorough history and physical exam, urgent diagnostic imaging should be performed. Plain radiographs are of limited value in the diagnosis of CES, but may be useful to evaluate for alternate pathology such as a fracture, dislocation or subluxation, tumor, or infection. Diagnosing lumbar disc herniation in CES requires a CT or MRI. MRI is the gold standard for evaluating patients because it allows for detailed visualization of the spinal canal, disc spaces, nerve roots, and visualization of any potential space-occupying lesion within the canal or foramina. If MRI is contraindicated or unavailable, CT myelogram is the next best study to evaluate for CES. In addition to confirming the diagnosis, advanced imaging is helpful for preoperative planning for decompression.
TREATMENT AND OUTCOMES
In patients without absolute medical contraindications, CES is treated with emergent surgical exploration and nerve root decompression. A variety of surgical procedures and techniques are performed in the treatment of CES, ranging from minimally invasive micro-discectomies to extensive multiple-level bilateral laminectomies, discectomies, and occasionally arthrodeses. No significant evidence, however, supports the superiority of any one procedure. It is generally thought that surgical decompression should occur within 24 to 48 hours of CES diagnosis to prevent further neurologic decline and to improve chances of recovery. There is evidence to suggest that patients treated more than 48 hours after diagnosis had significantly decreased odds of recovering complete sensory, motor, sexual, urinary, and rectal function.
COMPREHENSION QUESTIONS
26.1 A 63-year-old woman with a history of metastatic lung cancer, diabetes, and bradycardia requiring a permanent pacemaker presents with 24 hours of urinary retention and progressive bilateral lower extremity weakness, beginning spontaneously. What is the next step in management?
A. Metastatic workup including CT of chest and preparations for biopsy, if applicableB. High-dose intravenous methylprednisolone × 24 hours and short-term bedrestC. Administration of nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen, activity modification, physical therapy, and close follow-upD. Emergency CT myelogram of the lumbosacral spineE. Emergency MRI of chest with gadolinium contrast
26.2 A 55-year-old man presents with low back pain and right “foot drop” 72 hours after straining his back trying to shovel snow from his driveway. He denies bowel or bladder changes. Sensation is intact throughout his bilateral lower extremities and perianal region, with the exception of some numbness to light touch across the dorsum of his right foot. He has a weak extensor hallucis longus and tibialis anterior (3/5) on his right side, but otherwise full strength in his bilateral low extremities. Straight leg raise is positive on his right side, sending “electric shock” sciatic pain down to his foot. He takes warfarin for atrial fibrillation, and his international normalized ratio (INR) is 2.5. He has no additional symptoms, nor medical history. What is the next step in the management of this patient?
A. High-dose intravenous methylprednisolone for 24 hoursB. Emergency MRI, if not contraindicated, of lumbosacral spineC. NSAIDs, acetaminophen, activity modification, and physical therapyD. Urgent reversal of INR with vitamin K and/or fresh-frozen plasma and preoperative planning including making the patient nothing by mouth (NPO), acquiring preoperative laboratory studies, chest x-ray, and electrocardiogram (ECG)E. Epidural steroid injection
26.3 A 44-year-old woman suffers a fall while rock climbing, landing on her buttocks and falling forward. Despite prolonged airlift to the ED, she is hemodynamically stable. She complains of bilateral pain in her legs, distal to her knees. She has profound weakness in her bilaterally extensor hallucis longi and gastrocsoleus complexes and has marked saddle anesthesia. MRI shows a large, midline herniated disc, compressing each of the traversing nerve roots and entire cauda equina below its level, but sparing the exiting nerve roots. Which disc is most likely involved in this injury?
A. L2-3B. L3-4C. L4-5D. L5-S1E. S1-2
ANSWERS
26.1 B. This patient has acute symptoms of CES. Although MRI of the lumbosacral spine is the ideal study to confirm this diagnosis, this patient’s pacemaker may be a contraindication to MRI. In such situations, CT myelography is the next best option. When performed for CES evaluation, MRIs should focus on the lumbosacral spine, not the chest and abdomen, and gadolinium contrast is usually unnecessary. Although steroids and/or NSAIDs and physical may play a role in treatment of acute HNP, they are not the first line in the treatment of CES. Likewise, this patient may require metastatic workup, but this is not the priority in the acute management of CES.
26.2 C. This patient’s history and presentation is consistent with an isolated, acutely HNP at L4-5. Although his motor and sensory deficits are concerning, the majority of patients will experience resolution of symptoms with nonoperative conservative management including NSAIDs, acetaminophen, physical therapy, and activity modification. Although an MRI may be helpful in making this diagnosis, it is not emergently indicated, as this patient does not have evidence of CES or other pathology that would require emergency, extensive workup, or surgical intervention. Epidural steroid injection is not the first line of treatment for an acute HNP, but may offer some relief in patients with refractory symptoms. Generally, epidural injection should not be performed with a significantly elevated INR.
26.3 C. This patient has weak extensor hallucis longi (L5 nerve root), weak gastrocsoleus complexes (S1), and saddle anesthesia (S2-4). She has normal function above this level, suggesting that the L5 nerve roots and those below are affected. An injury at L4-5 that spares the exiting roots (L4) but affects the traversing roots (L5) and those below (S1-5) would be most consistent with these symptoms. Remember the sacral spine does not have interbody discs, as it is fused.
CLINICAL PEARLS
► CES is defined by a characteristic cluster of symptoms, including low back pain, sciatica, lower extremity sensorimotor loss, and bowel and bladder dysfunction. ► CES is treated with urgent surgical decompression, unless there is an absolute contraindication to surgery. ► CES is a surgical emergency! Preparations for urgent operative intervention should begin as soon as the diagnosis is suspected. |
REFERENCES
Flynn, JM, ed. Lumbar degenerative disease. In: Orthopaedic Knowledge Update: Ten . Rosemont, IL: American Academy of Orthopaedic Surgeons; 2011:599-610.
Spector LR, Madigan L, Rhyne A, Darden B, Kim D. Cauda equina syndrome. J Am Acad Orthop Surg. 2008;16:471-479.

0 comments:
Post a Comment
Note: Only a member of this blog may post a comment.