Adult Acquired Flatfoot Deformity Case File
Eugene C. Toy, MD, Andrew J. Rosenbaum, MD, Timothy T. Roberts, MD, Joshua S. Dines, MD
CASE 35
A 47-year-old woman complains of pain at the medial side of her ankle. She works constantly on her feet as real estate agent. She says that she has had a relatively flatfoot her whole life, but it has worsened over the last 3.5 years and believes that the arch is collapsing. She says when she is in the shower it feels like the foot cups the floor. She also has a bunion that seems to have progressed over time. It is dramatically affecting her ability to walk and work. She has tried conservative care in the form of an orthotic and an ankle brace, but the condition continues to worsen her quality of life. On her exam, she has good ankle and subtalar range of motion. She has obvious increased heel valgus on the left side compared with the right. There is a sense of fullness and pain to palpation over the medial aspect of the ankle. On sitting, she can invert, evert, plantar flex, and dorsiflex the ankle with normal strength. However, on standing, she has increased foot abduction, and the arch appears to be collapsed. She cannot perform a single heel raise on the left side but can do so normally on the right side. She also has gastrocnemius tightness. The first ray is hypermobile.
► What is the most likely diagnosis?
► What imaging will help confirm the diagnosis?
► What is the surgical treatment of this condition?
ANSWER TO CASE 35:
Adult Acquired Flatfoot Deformity
Summary: A 47-year-old woman presents with medial ankle pain and worsening flat foot over the last 3.5 years. The patient has tried orthotics and an ankle brace. On exam, she has increased heel valgus, decreased arch, and inability to single heel raise, with pain over the medial aspect of the ankle.
- Most likely diagnosis: Adult acquired flatfoot deformity (AAFD; originally known as posterior tibial tendon insufficiency).
- Imaging: Initial plain radiographs of the foot should be obtained in a weightbearing stance, including an anteroposterior (AP) view to evaluate the talonavicular coverage angle and a lateral view to evaluate the first tarsometatarsal angle (Meary angle), the calcaneal pitch, and the alignment of the hindfoot. Additionally, radiographs of the ankle should be obtained to evaluate for the presence of a valgus tilt.
- Surgical treatment: Medializing calcaneal osteotomy with a flexor digitorum longus transfer to the navicular. Other accessory procedures depend on the nature of the deformity.
- Understand the pathophysiology behind the development of AAFD, and appreciate the bony, tendinous, and ligamentous anatomy implicated in its development.
- Understand the nonoperative approach to patients with AAFD.
- Appreciate the indications and purpose of each step in the algorithm for surgically treating AAFD.
Considerations
This 47-year-old woman has a history of a flatfoot that has worsened over time. The medial arch pain is most likely caused by inflammation and tenderness of the posterior tibial tendon. She has already failed a number of conservative treatments designed to maintain the foot in a more anatomic position. This includes the orthotic, which gives arch support and also tilts the heel out of the valgus position. Figures 35–1 , 35–2 , 35–3 , and 35–4 comprise a standard radiographic workup for AAFD. These radiographs demonstrate collapse at the medial arch (lateral view), a forefoot abduction deformity (AP view), and increased heel valgus (ankle AP and mortise views). An MRI is also very helpful and will show thickening of the posterior tibial tendon and failure of the ligaments of the medial arch. Surgical treatment can be performed after failure of conservative treatment. This consists of a variety of corrective osteotomies and tendon transfers in patients with flexible deformity as present in this patient. Patients with rigid deformity are better served with selective fusions of the hindfoot.

Figure 35–1. Mortise view plain radiograph of the left ankle. (Courtesy of Scott Ellis, MD)
Figure 35–2. Lateral foot plain radiograph showing a decreased pitch at the calcaneus and a
decreased first tarsometatarsal angle. (Courtesy of Scott Ellis, MD)
Figure 35–3. Anteroposterior plain radiograph of the left foot demonstrating increased forefoot
abduction through the talonavicular joint and the presence of a severe bunion (hallux valgus deformity).
(Courtesy of Scott Ellis, MD)
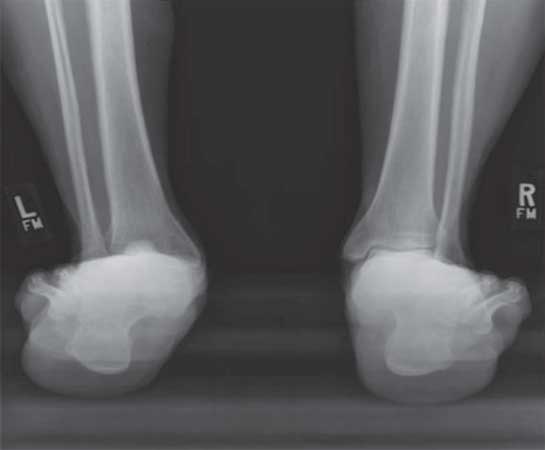
Figure 35–4. Hindfoot alignment view shows increased hindfoot valgus. (Courtesy of Scott Ellis, MD)
APPROACH TO:
Adult Acquired Flatfoot Deformity
DEFINITIONS
POSTERIOR TIBIAL TENDON: The major invertor of the hindfoot, which has its origin along the posterior aspect of the leg and its insertion on the navicular.
MEDIALIZING CALCANEAL OSTEOTOMY: Surgically cutting the calcaneal bone from the lateral side, which is used to translate the posterior portion of the bone attached to the Achilles in a medial fashion. The osteotomy is fixed by 2 screws passed axially up the long axis of the heel bone or calcaneus.
FLEXOR DIGITORUM LONGUS TRANSFER: A surgical rerouting of the tendon, which normally attaches to the plantar surface of the base of the distal phalanges of the 4 lesser toes, to the navicular to replace or enhance the action of the posterior tibial tendon.
GASTROCNEMIUS RECESSION: This is a selective lengthening of the fascia just distal to the muscle body of the gastrocnemius that does not compromise the soleus muscle and therefore lengthens the Achilles complex in a modest fashion.
LATERAL COLUMN LENGTHENING: A surgical cut of the anterior/lateral aspect of the calcaneus that is used to place a graft and move the forefoot out of relative abduction.
SPRING LIGAMENT: The calcaneonavicular ligament, which is a sleeve of tissue that extends from the calcaneus to the navicular and helps support the talar head.
DELTOID LIGAMENT: The ligament connecting the medial malleolus to the talus and calcaneus that helps to prevent the ankle joint from tilting into valgus.
ARIZONA BRACE: A brace that incorporates a custom-made orthotic with a lace-up ankle brace used to help control adult acquired flatfoot deformity.
HINDFOOT VALGUS: A malalignment of the heel with its base displaced laterally when viewed from behind.
FOREFOOT ABDUCTION: A relative position of the toes further away from the midline of the body than normal.
CLINICAL APPROACH
Etiologies
The true cause of the AAFD is not known. Generally, however, it is thought to occur more commonly in women, particularly those who are ligamentously lax and in those who are overweight, which places more strain on the posterior tibial tendon. This tendon goes on to stretch and fail along with the ligaments that support the arch, including the spring ligament. Patients generally complain of having a flatfoot their whole life, which worsens over time. It is thought that the hypovascular nature of the tendon in the area of failure is a leading cause. This generally occurs in women beginning in their fifties.
Clinical Presentation
Most patients present first with pain in the medial arch area. This corresponds with the area of the posterior tibial tendon. They also note a decrease in the arch and the position of their heel in more valgus. The foot generally begins to feel weaker. As the disease progresses, pain may shift laterally. This is commonly because the heel begins to impinge underneath the fibula.
The physical exam shows the patient to have a decreased arch with the heel positioned in valgus. Patients commonly have an abducted forefoot. A helpful diagnostic test is the single heel raise. Patients with posterior tibial tendon insufficiency are unable to raise their heel from the ground or, if they can do so, are not able to fully invert the heel. Patients also commonly present with a bunion and a tight gastrocnemius muscle, which occurs as the heel moves in the more relative position of valgus and shortens the Achilles.
Diagnosis
The diagnosis is commonly made based on the history. The inability to perform a single heel raise is very suggestive as well. Radiographs indicate the location and amount of deformity ( Figures 35–1 , 35–2 , 35–3 , and 35–4 ). On a lateral x-ray, patients have a decreased first tarsometatarsal angle showing collapse on the inside arch. The hindfoot alignment view generally shows that the heel is in relative position of valgus. AP x-rays show that the navicular bone moves lateral relative to the talus, which suggests that there is forefoot abduction. An MRI can be helpful as well, which shows not only enlargement and degeneration of the posterior tibial tendon, but also failure of the spring ligament complex.
Once the diagnosis of AAFD is made, it can be classified. Classification into 4 stages of severity helps guide treatment and prognosis. In stage I, the foot and ankle are without deformity, however there maybe pain from posterior tibial tendinosis. In stage II, the flatfoot deformity is apparent, but it is flexible throughout, meaning, the examiner can pull it into appropriate alignment. In stage III, the flatfoot deformity becomes rigid and is uncorrectable by manipulation. Finally, by stage IV, there is an additional rigid valgus tilt to the ankle due to compromise of the deltoid ligament.
TREATMENT
Treatment depends on the stage of the deformity. In general, those with stage I or no deformity can be treated conservatively with an orthotic and relative rest. Patients with stage II deformity generally are first approached with an orthotic, which gives arch support, and a medial post, which is used to raise the inside aspect of the heel and tilt the heel out of valgus. An ankle brace that is usually a lace-up or velcro brace can be used to help stabilize the hindfoot. Commonly, patients must go on to try an Arizona brace, which is a custom-made orthotic built in with an ankle brace. Patients with stage III AAFD respond less favorably to orthotics and bracing given that the deformity is rigid and not correctible. Stage IV generally also requires more aggressive treatment, given the collapse that is occurring through the ankle unless the patient is relatively asymptomatic.
Surgical treatment also depends on the stage. Surgery is rarely indicated for patients without deformity or stage I. In stage II, a medializing heel slide is commonly performed, along with a transfer of the flexor digitorum longus tendon to the navicular. If the posterior tibial tendon is very diseased, it can be resected. A gastrocnemius resection, lateral column lengthening, and medial column procedures such as first tarsometatarsal fusion or osteotomy to the medial cuneiform (Cotton osteotomy) can be also used. For stage III deformity, a fusion of the triple joint complex, which includes the subtalar, talonavicular, and calcaneal cuboid joint, must be performed. In stage IV, the ankle must be addressed concomitantly with the foot either through trying to reconstruct the deltoid, performing an ankle fusion, or performing ankle replacement.
COMPREHENSION QUESTIONS
35.1 Which of the following best defines the “spring ligament”?
A. Talocalcaneal ligament
B. Calcaneonavicular ligament
C. Talonavicular ligament
D. Calcaneofibular ligament
35.2 Which of the following best describes the action of the posterior tibial tendon?
C. Plantar flex the ankle
35.3 A 55-year-old woman presents with a severe flatfoot deformity with arthritis in the subtalar joint. On exam, she has increased hindfoot valgus and forefoot abduction, which is not correctable on physical exam. Which stage is this flatfoot deformity?
35.4 A 60-year-old man presents with a 2-year history of medial ankle pain and a severe flatfoot deformity, which is correctable on physical exam. Which of the following best describes the orthotic that may be used to help treat this deformity?
A. Lateral posting and a first metatarsal well
B. Lateral posting with a metatarsal pad
C. Medial heel posting with arch support
D. A carbon-graphite insert with an extension to protect the great toe
35.5 A 52-year-old woman who is moderately obese and who has had flatfoot deformity her whole life is now presenting with worsening hindfoot pain, particularly around the medial aspect of her ankle. She has increased heel valgus on exam with forefoot abduction and a decreased arch. She cannot perform a single heel raise. MRI confirms a decreased arch and posterior tibial tendinosis. Which of the following best describes the surgical treatment?
A. Lateralizing heel slide and a flexor digitorum longus transfer to the navicular
B. Lateralizing heel slide and a deltoid ligament repair
C. Medializing heel slide with lateral column shortening through the anterior calcaneus
D. Medializing heel slide with a flexor digitorum longus transfer to the navicular
ANSWERS
35.1 B. The spring ligament connects the calcaneus and navicular, holding up the talar head and helping support the medial arch.
35.2 D. The posterior tibia tendon inserts on the navicular. Its primary action is to invert the hindfoot and can be assessed with the single heel raise test.
35.3 C. A flatfoot deformity that does not correct on exam is considered rigid and therefore classified as stage III. Arthritis is commonly present.
35.4 C. A medial heel post helps tilt the heel out of valgus. The arch support helps to maintain the medial arch. Metatarsal posts are generally used for pain under the metatarsals, and the carbon-graphite insert above is generally used for patients with arthritis in the great toe joint.
35.5 D. The heel must be cut and translated medially to bring the calcaneus out of valgus. The flexor digitorum transfer to the navicular helps restores inversion power to the foot.
CLINICAL PEARLS
►AAFD usually is caused by failure of the ligaments supporting the medial arch along with the posterior tibial tendon.
► Patients with AAFD present with hindfoot valgus and an inability to do a single heel raise.
► Standard weightbearing radiographs often diagnose flatfoot deformity due to decreased first tarsometatarsal angle on a lateral view, increased forefoot abduction through the talonavicular joint on an anteroposterior view, and a hindfoot alignment view showing increased heel valgus.
► MRI can also show the failure of the posterior tendon and medial arch ligaments.
► Conservative treatment generally consists of orthotics and bracing.
► Surgical reconstruction usually consists of an osteotomy of the calcaneus and a tendon transfer in the foot in patients with flexible deformity.
|
REFERENCES
Deland JT. Adult-acquired flatfoot deformity. J Am Acad Orthop Surg. 2008;16:399-406.
Deland JT, Page A, Sung IH, O’Malley MJ, Inda D, Choung S. Posterior tibial tendon insufficiency
results at different stages. HSS J. 2006;2:157-160.
Haddad SL, Myerson MS, Younger A, Anderson RB, Davis WH, Manoli A 2nd. Symposium: adult
acquired flatfoot deformity. Foot Ankle Int. 2011;32:95-111.
Johnson KA, Strom DE. Tibialis posterior tendon dysfunction. Clin Orthop Relat Res. 1989:196-206.
Myerson MS. Adult acquired flatfoot deformity: treatment of dysfunction of the posterior tibial tendon.
Instr Course Lect. 1997;46:393-405.
Younger AS, Sawatzky B, Dryden P. Radiographic assessment of adult flatfoot. Foot Ankle Int. 2005;26:
820-825.




0 comments:
Post a Comment
Note: Only a member of this blog may post a comment.