Osteomyelitis Case File
Eugene C. Toy, MD, Andrew J. Rosenbaum, MD, Timothy T. Roberts, MD, Joshua S. Dines, MD
CASE 20
A 62-year-old female is referred to your office for a 3-week history of right foot pain. The patient denies recent trauma to the area, but states she had her second toe amputated by her podiatrist 6 months ago, secondary to an infection she contracted “from a pebble in [her] shoe.” Although her foot had healed, she has begun experiencing a recurrence of pain in this area, despite a change in footwear and diligent monitoring of her feet for ulcers. She admits to mild fevers over the past 10 days, but denies other symptoms. On further history, the patient has type 2 diabetes mellitus. She admits that she stopped seeing her primary care physician last year since he started prescribing “painful insulin shots” for her. On physical exam, erythema is noted at the plantar-medial aspect of her right forefoot. This region is warm to the touch, mildly edematous, and firm, but without any obvious fluctuance or drainage. She has chronic neuropathies in her toes and feet, bilaterally. Recent laboratory results from her primary care provider’s office are remarkable for a white blood cell (WBC) count of 7.4 thousand/μL, erythrocyte sedimentation rate (ESR) of 55 mm/hr, and C-reactive protein (CRP) of 65 mg/L. An anteroposterior (AP) x-ray and a T2-weighted magnetic resonance imaging (MRI) of the right foot are shown in Figures 20–1 and 20–2 .
► What are the radiologic findings?
► What is the most likely diagnosis?
► What risk factors predispose her to such a diagnosis?
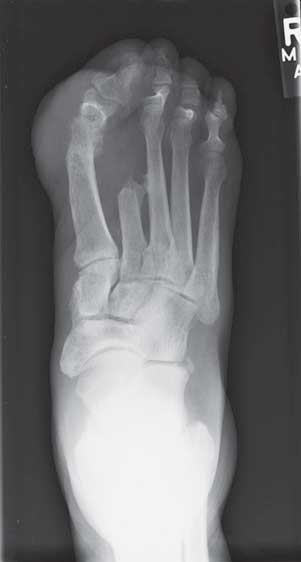
Figure 20–1. AP radiograph of the right foot, status post second ray resection.
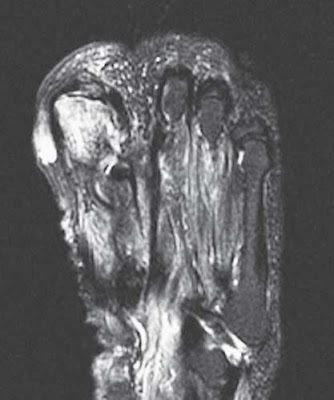
Figure 20–2. T2-weighted axial MRI slice of the right foot.
ANSWER TO CASE 20:
Osteomyelitis
Summary: A 62-year-old woman with uncontrolled diabetes and peripheral neuropathy presents with atraumatic, insidious right foot pain, 3 weeks in duration. She has mild systemic symptoms (fever) and has experienced similar symptoms in the past for which she underwent an amputation of her second toe.
- Radiologic findings: This AP radiograph of the right foot shows chronic bone and soft tissue loss in the second ray, consistent with the patient’s history of osteomyelitis and toe amputation. There is significant soft tissue swelling over the head of the first metatarsal and base of the great toe. There is also significant bony erosion in this region, with a loss of normal cortical bone, periosteal elevation, and lytic changes consistent with osteomyelitis. On T2-weighted MRI, the head and distal shaft of the first metatarsal are hyper-resonant, consistent with edema and inflammation in the region. There is also adjacent hyperintensity of the soft tissues medial to the great toe, consistent with soft tissue inflammation and possibly an abscess collection.
- Most likely diagnosis: Osteomyelitis of the first ray.
- Predisposing factors: Poorly controlled type 2 diabetes mellitus, peripheral neuropathy, and history of previous osteomyelitis.
ANALYSIS
Objectives
- Understand the pathogenesis of osteomyelitis and recognize its clinical and radiographic presentation.
- Be familiar with the differential diagnoses for, and diagnostic workup of, osteomyelitis.
- Be familiar with basic treatment options for osteomyelitis, both operative and nonoperative.
Considerations
This patient presents with a soft tissue infection that has progressed to involve the underlying metatarsal bone. She has a history of uncontrolled diabetes and neuropathy. As a risk factor for osteomyelitis, neuropathies predispose patients to microtrauma because the body’s pain-protective response to skin-damaging repetitive wear is lost. Previously, this patient’s neuropathy left her susceptible to skin ulceration from a pebble in her shoe, which wore through the protective dermal barrier and introduced bacteria into the soft tissues overlying the second metatarsal. Poorly controlled diabetes impedes the body’s wound healing and infection-fighting capabilities, rendering diabetics susceptible to bacterial colonization, particularly in their feet. Radiographic studies should be used to further investigate and diagnose osteomyelitis: plain radiographs, computed tomography (CT) scans, MRI, WBC scans, and/or bone scans are used to make the diagnosis. In this patient’s case, plain x-rays clearly show erosive bony changes in the first ray, while T2-weighted MRI shows edematous changes in the bone and surrounding soft tissues consistent with osteomyelitis. This patient has an elevated ESR and CRP, which are elevated in more than 90% of cases of osteomyelitis. An elevated WBC count, although positive in many types of infections and inflammatory states, is only positive in approximately 40% of cases.
Once the diagnosis is made, the patient should be admitted to the hospital and intravenous antibiotic therapy should commence. If deep tissue or bone biopsy can be easily obtained, and if the patient remains stable, antibiotic therapy may be delayed until biopsies or aspirations are acquired. This is especially true in patients for whom osteomyelitis represents one in several possible diagnoses or when
osteomyelitis is occurring in particularly difficult to debride regions such as vertebral bodies. Biopsy before antibiotic administration optimizes the chance that an adequate sample of bacteria will be acquired for culture and that an appropriate, targeted antibiotic agent may be selected. Unstable patients with evidence of sepsis, however, should receive prompt systemic antibiotic treatment, regardless of whether biopsy can be performed. An additional caveat involves the culturing of superficial tissues, as these cultures tend to grow out benign, typical skin flora, which sometimes leads to the unnecessary and misdirected treatment.
For this patient, with extensive involvement of deep tissues, surgical drainage and debridement should be performed. Amputation may also be considered. Intravenous antibiotic therapy typically continues for 4 to 6 weeks, with infectious disease consultation useful for assistance with antibiotic selection and management.
APPROACH TO:
Osteomyelitis
DEFINITIONS
ACUTE OSTEOMYELITIS: Presence of bacteria or infectious pathogens in bone or bone marrow without the chronic histologic changes described below. Defined in some literature as a bone infection lasting less than 6 weeks. Acute osteomyelitis most commonly occurs in children.
CHRONIC OSTEOMYELITIS: May be defined by histologic changes such as the presence of a sequestrum or an involucrum, or by duration of infection greater than 6 weeks. Chronic osteomyelitis is characterized by the presence of bacterial biofilm and bacterial resistance to host defenses and antibiotic agents and often requires surgical debridement and long-term systemic antibiotic therapy.
BIOFILM: An aggregate of microorganisms embedded within an adherent polysaccharide matrix that provides bacterial immunity to host cellular defenses and antiobiotic agents.
SEQUESTRUM: A region of devitalized bone that serves as a nidus for continual infection; a hallmark of chronic osteomyelitis.
INVOLUCRUM: The formation of new, reactive bone around an area of septic necrosis; another hallmark of chronic osteomyelitis.
CLINICAL APPROACH
Pathophysiology
Osteomyelitis is an infection of bone or bone marrow. This highly variable disease may be classified as acute versus chronic, hematogenous versus contiguous, and with or without vascular compromise (Lee and Waldvogel classification). Osteomyelitis may also be classified by its location and extent (Cierny and Mader classification).
Osteomyelitis can result from a continuous spread of an infection from soft tissue or joints, trauma causing direct bacterial inoculation into bone or adjacent soft tissues, or hematogenously spread from an infection elsewhere in the body.
Patients with vascular diseases, poorly controlled diabetes, and those in states of immunocompromise are at elevated risk for developing acute osteomyelitis. Immunocompromised individuals are also at risk for developing chronic osteomyelitis. Other risk factors for chronic osteomyelitis include history of intravenous drug abuse and failure of treatment of acute osteomyelitis.
Osteomyelitis can be caused by bacteria, fungi, and viruses. By a great majority, the most common causative agents are bacterial, with Staphylococcus aureus being the most commonly identified offending organism. Other common inoculants include Pseudomonas aeruginosa, Escherichia coli, coagulase-negative staphylococci, enterococci, and propionibacteria. Salmonella species are commonly identified pathogens in patients with sickle-cell anemia; however, staphylococcal species are still most common in these patients.
Diagnosis
Osteomyelitis may present as an occult infection in patients of all ages. Its most common presentation is in patients with deep bone pain and without significant systemic symptoms. When systemic symptoms are present, fever and chills predominate. Soft tissues surrounding an infection may be edematous, warm, and erythematous. Patients may present with a history of recent trauma or infection or with a history of an invasive procedure. Osteomyelitis should be included in the differential diagnosis of other musculoskeletal pathologies such as gout, ischemia, arthritis, neuropathy, and degenerative disc disease in the spine. Delay in diagnosis and treatment of acute infection may lead to chronic osteomyelitis, a relapsing and remitting indolent infection characterized by intermittent pain attacks and systemic symptoms.
Radiographic Evaluation
Plain radiographs should be obtained before more advanced imaging is considered. On plain films, acute osteomyelitis may be identified by cortical bone destruction with a surrounding area of periosteal elevation. Acute osteomyelitis will typically have a lytic, or radiolucent, appearance, whereas chronic infections may be distinguished by the presence of a mixed lytic and blastic, or radio-opaque, appearance. Radiographs are not sensitive for osteomyelitis, however, as up to 30% to 40% of bone destruction must occur before osteomyelitic changes are visible on plain x-rays. Symptoms of the disease typically are present before x-ray changes are apparent.
MRI with intravenous (IV) gadolinium contrast is far more sensitive for diagnosing osteomyelitis. MRI offers a clear view of soft tissue pathology and is currently the gold standard in the diagnosis of osteomyelitis. Be wary that in the presence of metallic implants, the sensitive/specificity of MRI is decreased; in such situations, IV contrast CT scans may be helpful in elucidating bony pathology.
Finally, radioisotope tagged WBC scans are very specific for osteomyelitis and are often used to follow treatment progression. Bone scans may be used in a similar fashion, but are less specific.
TREATMENT
Acute osteomyelitis, typically presenting in children and IV drug abusers with erythematous and painful limbs, requires prompt antibiotic therapy, often 4 to 6 weeks’ duration. Such patients may not require surgical debridement, but should be followed closely to ensure successful therapy.
Chronic osteomyelitis also requires long-term IV drug therapy, but typically requires additional open surgical procedures to debride necrotic tissue, drain abscesses, and remove sequestra or nonviable bone serving as nidi for bacteria.
In chronic osteomyelitis, IV antibiotic is typically administered for 4 to 6 weeks and may be administered in an outpatient setting once a patient has been stabilized. In patients with extensive disease or immunocompromised states, longer courses of IV drug therapy may be indicated. Initial antibiotic coverage should be broad, with tailored antibiotic selection once, and only if, reliable bacterial cultures and drug sensitivities are available. Initial antibiotic selection must cover S. aureus , the most commonly identified pathogen in osteomyelitis. In patients with a history of recent hospitalization, initial therapy must cover methicillin-resistant S. aureus, a prevalent nosocomial infection. Serial CRP and ESR studies, although not especially specific for osteomyelitis, are sometimes followed as markers for successful treatment.
In addition to a thorough surgical debridement, several adjunctive surgical treatments may be indicated, including the placement of antibiotic-eluting polymethyl- methacrylate (PMMA) beads. PMMA, the same bone “cement” used in the implantation of joint prostheses, may be mixed with antibiotic agents such as gentamycin, molded into round beads or fashioned into an antibiotic spacer, and placed into the debrided cavity. After resolution of infection, the beads are typically removed.
The placement of orthopaedic implants such as screws, plates, rods, and prostheses pose a special challenge to the orthopaedist, as artificial implants may serve as a nidus for chronic infection. In such cases, the surgeon must weight the benefits of removing infected hardware with the risks of losing stability or function. As a general rule, infected hardware should be removed when possible.
Outcomes and Complications
Musculoskeletal infection that has been treated with antibiotics and surgical debridement can lead to functional deficit in the given extremity. This is dependent on the amount of tissue debrided and if vital structures have been violated and destabilized. When this occurs, it is usually in an attempt to perform a limb-salvage procedure, as both patients and surgeons try to avoid amputation if at all possible. However, in the setting of severe and recurrent musculoskeletal infections, amputation may be the only means by which to permanently eradicate the infection.
COMPREHENSION QUESTIONS
20.1 A 34-year-old, HIV-positive male presents to the emergency department (ED) with complaints of several weeks of neck pain. The patient admits to using recreational drugs, but does not willingly discuss what substances he uses. He has recently begun feeling numbness in his bilateral hands and states he is now unable to properly write with a pen. On exam, he has point tenderness along the lateral aspect of his neck. An MRI is obtained, showing edema and prevertebral swelling in his C3 and C4 vertebrae. There is T2-weighted hyperresonance of the C3-4 disc space, with swelling posterior to C3 that is impinging on the cord. What is the best treatment for this patient?
A. Inform the patient that he should follow up as an outpatient for further workup.B. Physical therapy and warm compresses, as the patient has no symptoms of myelopathy.C. Admit to the hospital promptly for antibiotic therapy and evaluation for surgical intervention.D. Bone scan and CT scanning of the chest abdomen and pelvis to evaluate for other lesions.E. Biopsies to classify the lesions and determine their source.
20.2 A 44-year-old truck driver is almost 1 year in recovery from knife wound to his left distal thigh after an altercation at a local bar. He had initially been treated with debridement in the ED and wound closure and was treated with a short course of oral antibiotics. He was neurovascularly intact after the injury. He presents now to your clinic with serous drainage through a sinus tract on the medial aspect of his distal thigh. The area is erythematous and edematous and is mildly tender to palpation. He has been able to bear weight on it, but states that it is causing increasing discomfort while trying to drive his truck. Plain radiograph films are obtained and are equivocal. An MRI is also obtained and shows a region of hyperintensity in the metaphysis of the distal left femur surrounding an area of hypointense bone. What is the best treatment for this patient?
A. Long (14-day) course of oral antibiotics with close follow-upB. Needle biopsy and targeted oral antibioticsC. CT scan of the affected extremityD. Needle biopsy and IV antibioticsE. Surgical debridement and IV antibiotics
20.3 A 12-year-old African American male with a history of sickle cell disease is admitted to the hospital with severe left upper extremity pain and fevers. Blood cultures are obtained, and broad-spectrum IV antibiotics and fluid resuscitation are initiated. What is the most likely causative organism in this patient?
A. Viral infectionB. SalmonellaC. Streptococcus speciesD. Staphylococcus aureusE. Escherichia coli
ANSWERS
20.1 C. This patient has osteomyelitis of the cervical spine with discitis at C3-4, and evidence of epidural abscess. Given the patient’s myelopathic state, the patient should be admitted immediately to the hospital and IV antibiotic therapy should begin promptly, ideally after a biopsy is obtained. If symptoms do not remit on broad-spectrum antibiotic treatment, or if myelopathy worsens, prompt surgical evacuation of the abscess should be performed.
20.2 E. This patient has history and radiographic findings consistent with a chronic osteomyelitis. The region of bone involved on MRI is consistent with a sequestrum that must be surgically debrided. After culture, broad-spectrum IV antibiotics should be initiated and targeted according to susceptibility testing of the cultures. Although needle biopsy may help target the appropriate organism, it is insufficient to effectively eradicate the infection. Similarly antibiotics alone, whether oral or broad-spectrum IV, are insufficient without a thorough surgical debridement.
20.3 D. Although Salmonella species are commonly associated with sickle cell patients with osteomyelitis, the most common causative agent is actually S. aureus. Escherichia coli and streptococcal species infections also occur in these populations; however, they are less common. Viral osteomyelitis is exceedingly rare.
CLINICAL PEARLS
► Osteomyelitis is sometimes referred to as the “great imitator” because it can radiographically mimic almost any neoplastic or inflammatory process. ► Osteomyelitis must destroy 30% to 40% of a given region of bone before it is evident on plain x-ray. ► Elevated WBC counts are found in only 40% of patients presenting with chronic osteomyelitis; elevated CRP and ESR are found in approximately 90%. ► Acute osteomyelitis usually requires prolonged IV antibiotic therapy. Chronic osteomyelitis generally requires surgical debridement as well as prolonged antibiotics. |
REFERENCES
Forsberg JA, Potter BK, Cierny III G, Webb L. Diagnosis and management of chronic infection. J Am Acad Orthop Surg. 2011;19(suppl 1):S8-S19.
Frassica FJ, Frassica DA, McCarthy EF. Orthopaedic pathology. In: Miller MD, ed. Review of Orthopaedics . 5th ed. Philadelphia, PA: Saunders Elsevier; 2008.
Srinivasan RC, Tolhurst S, Vanderhave KL. Orthopedic surgery. In: Doherty GM, ed. Current Diagnosis & Treatment: Surgery . 13th ed. New York: McGraw-Hill; 2010.
Tice AD. Osteomyelitis. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson JL, Loscalzo J, eds. Harrison’s Principles of Internal Medicine . 18th ed. New York: McGraw-Hill; 2012.

0 comments:
Post a Comment
Note: Only a member of this blog may post a comment.